Health communication
CONTENTS
Nutritional Management in Gout
1. Overview of Gout
Gout is a metabolic disorder associated with elevated levels of uric acid in the blood, known as hyperuricemia. When uric acid accumulates beyond its solubility threshold, monosodium urate crystals may deposit in the joints and surrounding tissues, leading to acute inflammation, pain, and swelling.
An acute gout attack commonly affects one or several joints. The most frequently involved sites include the first metatarsophalangeal joint, commonly known as the big toe, as well as the knees and ankles. The pain usually develops suddenly, often at night, and is typically described as severe, sharp, and throbbing. The affected joint may become red, warm, swollen, and extremely tender.
Most cases of gout result from reduced renal excretion of uric acid, which may occur in patients with chronic kidney disease or in those using certain medications such as diuretics. A smaller proportion of cases are caused by excessive uric acid production, which may be related to genetic enzyme abnormalities or conditions with increased cell turnover, such as psoriasis, polycythemia, or leukemia. However, not all individuals with hyperuricemia develop gout. In fact, many people with elevated serum uric acid remain asymptomatic.
2. Risk Factors
Several factors contribute to the development of gout. Age is an important factor, as the incidence of gout increases progressively over time. Sex also plays a role; younger men are more likely to develop gout than women, partly because estrogen promotes urinary urate excretion. Family history may increase susceptibility, suggesting a genetic component.
Dietary habits are strongly associated with gout risk. A high intake of purine-rich foods, such as red meat, organ meats, and seafood, can increase uric acid levels. Alcohol consumption, particularly beer, is also an important risk factor. Obesity and metabolic disorders further increase the likelihood of hyperuricemia and gout. In addition, medications such as diuretics, cyclosporine, low-dose aspirin, and niacin may raise serum uric acid levels. Stress, trauma, and surgery may also trigger acute gout attacks in susceptible individuals.

Figure 1. Foods that may increase serum uric acid levels.
3. Diagnosis
Although acute monoarthritis may suggest gout, diagnosis should not rely on symptoms alone. The most definitive diagnostic evidence is the identification of intracellular monosodium urate crystals in synovial fluid or in aspirated material from tophi. These crystals typically appear needle-shaped under microscopic examination.
Serum uric acid measurement can support the diagnosis, but it should be interpreted carefully because some patients may have normal uric acid levels during an acute attack. A 24-hour urinary uric acid test may help distinguish between uric acid overproduction and reduced excretion. In the early stages of gout, joint X-rays may appear normal. However, in long-standing or poorly controlled disease, characteristic bone erosions may develop.
4. Pharmacological Treatment
The treatment of gout includes two main goals: controlling acute inflammation and reducing long-term serum uric acid levels.
For acute gout attacks, nonsteroidal anti-inflammatory drugs, such as indomethacin, diclofenac, ibuprofen, and naproxen, are commonly used to reduce pain and inflammation. Corticosteroids may be indicated in patients with severe symptoms or in those who cannot tolerate NSAIDs, particularly individuals with renal impairment. Colchicine is another option, especially when NSAIDs or corticosteroids are contraindicated or ineffective.
For long-term uric acid control, urate-lowering therapy may be required. Allopurinol and febuxostat reduce uric acid production by inhibiting xanthine oxidase. Probenecid increases renal uric acid excretion but may raise the risk of kidney stones. Losartan, an antihypertensive medication, may also reduce uric acid levels by inhibiting urate reabsorption. In severe cases, especially when tophi cause joint deformity, persistent pain, or nerve compression, surgical intervention may be considered.
5. Nutritional Management in Gout
Nutrition plays an important supportive role in the prevention and management of gout. Since uric acid is produced from purine metabolism, reducing the intake of purine-rich foods can help lower the risk of recurrent gout attacks.
Patients with gout are generally advised to limit red meat, organ meats, and certain types of seafood. Instead, low-purine foods such as low-fat milk, white cheese, bread, cereals, rice, potatoes, fruits, and vegetables are recommended. Plant-based protein sources, including legumes, may be used as alternatives to animal protein. Although some plant foods contain purines, they appear to have a lower impact on serum uric acid compared with meat and seafood. In addition, certain compounds found in legumes, such as flavonoids, may have inhibitory effects on xanthine oxidase activity.
Maintaining a healthy body weight is also essential. Obesity is strongly associated with an increased risk of gout, and the risk rises progressively with higher body mass index. However, rapid weight loss or extreme dieting should be avoided, as these may temporarily increase uric acid levels and trigger gout attacks.
Alcohol intake should be restricted, particularly beer. Ethanol metabolism increases purine breakdown and uric acid production. Beer has the strongest association with gout risk because it contains both alcohol and purine-rich components. Sugary beverages should also be limited, especially those containing fructose. Fructose can increase uric acid production and may contribute to insulin resistance, which reduces renal uric acid excretion.
Adequate hydration is important, especially because gout increases the risk of kidney stone formation. Drinking more than two liters of water per day may help reduce this risk. Vitamin C supplementation has also been shown in some studies to reduce serum uric acid levels by promoting renal excretion, although supplementation should be considered as a supportive measure rather than a replacement for medical treatment.
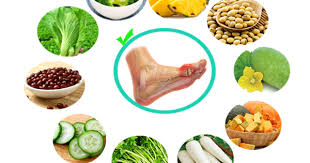
Figure 2. Recommended foods for patients with gout.
6. Conclusion
Gout is a chronic metabolic disease closely related to hyperuricemia, renal uric acid handling, lifestyle factors, dietary habits, obesity, and medication use. While pharmacological treatment is necessary for controlling acute attacks and maintaining target uric acid levels, nutritional management remains an important component of long-term disease control.
A scientifically appropriate diet for gout should focus on limiting purine-rich animal foods, reducing alcohol and fructose-containing beverages, maintaining a healthy body weight, increasing water intake, and choosing low-purine, nutrient-rich foods. These measures can help lower uric acid levels, prevent recurrent gout attacks, and improve overall disease management.
References
- MedlinePlus. Gout. MedlinePlus Medical Encyclopedia. Reviewed April 1, 2025. Accessed April 25, 2026.
- Barnard, N. D. (Ed.). Gout. In Nutrition Guide for Clinicians (3rd ed.). Physicians Committee for Responsible Medicine; 2024. Accessed April 25, 2026.
- Kim Ngoc Son, MSc;
- Pham Xuan Khoi, MSc.

